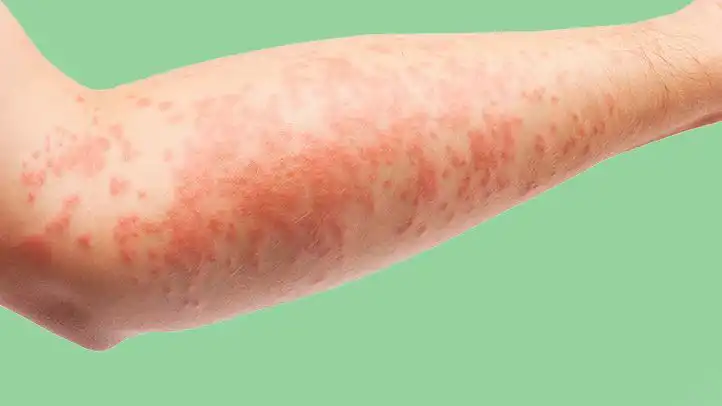
Urticaria is a disorder of the skin commonly referred to as “hives”. It is a skin rash notable for pale red, raised, itchy bumps that also can cause a burning or stinging sensation. There are several classifications of urticaria depending on how it presents, as well as the duration of the rashes. In simple terms urticaria can be broken down into acute and chronic types.
Acute urticaria is often from foods, medications, or skin contact with chemicals. The hives usually come on quickly and disappear within 24 hours or so. The inflammatory immune chemical known as histamine can often be a culprit in acute urticaria. If a person has a ‘food sensitivity’ then the white blood cells (basophils) of the immune system can create the inflammatory chemical histamine in response to the food antigen. Some people have trouble clearing the histamine contributing to the symptoms of acute urticaria. Foods naturally high in histamine can also cause symptoms. High histamine foods include anything that is aged, seafood, fermented or leftover in the fridge.
Histamine intolerance is often because the body cannot make adequate amounts of Diamine Oxidase (DAO) which is an enzyme that breaks down the histamine. DAO is made in the small intestine, but many people seem to be lacking adequate production to reduce the overall histamine load. People can often control their acute urticaria by taking the enzyme DAO in pill form which will break down histamine. Or they can modify their diet to reduce their intake of histamine containing foods. If someone has acute urticaria and migraines I would absolutely consider a trial of DAO to see if it symptoms improve.
Chronic urticaria is also an allergic skin condition similar to acute urticaria, but lasts more than 6 weeks. As opposed to acute urticaria which can come and go, the chronic form can stick around and is often related to autoimmune diseases. Chronic urticaria is often difficult to treat as there are many symptoms and the conditions appears so ‘deep’. The cause is currently unknown and allopathic treatment options are limited to anti-inflammatory medications. However a study was just released showing that Vitamin D supplementation can be a useful adjunct therapy for the chronic condition.
This Vitamin D study had 38 participants who were afflicted with chronic hives from 5 to 20 years. Over a 3 month period subjects took a daily triple-drug combination of allergy medications (one prescription and two over-the-counter drugs) and one vitamin D3. In addition to the medication, 18 of the patient’s took 600 IUs of vitamin D3 and the other 18 took 4000 IUs. After just one week, the severity of patients’ symptoms decreased by 33 percent for both groups. But at the end of three months, the group taking 4000 IUs of vitamin D3 had a further 40 percent decrease in severity of their hives. The low vitamin D3 treatment group had no further improvement after the first week.
This last sentence flies in the face of the laughable recommendation by the Institute of Medicine (IOM) Nutrition Board that 600IU of Vitamin D/day are adequate. There is plenty of excellent evidence that at least 4000IU/day or more are beneficial for many people, especially during winter months at latitudes such as New England. Unfortunately the study did not provide the vitamin D levels of the subject prior to testing, however a study released in the beginning of February did show that Vitamin D is low in chronic urticaria patients compared to the general population.
Vitamin D plays an enormous role in modulating our immune system. In addition, skeletal, skin, bone marrow, brain, colon, breast cells all contain Vitamin D Receptors (VDR). This means that vitamin D can modulate many aspects of our physiology. The correct amount for each person is different. Perhaps the IOM’s recommendation of 600IU/day is great for a healthy person, but if there is any underlying dis-ease then more is needed. In the above study the group receiving 600IU/day had the same benefit as the 4000IU/day group in the short term.. However long term the 4000IU/day group showed an additional 40% decrease in urticaria symptoms. It seems at least in some disease states higher doses of Vitamin D confers extra benefit to have lasting physiological benefit.
This doesn’t mean that everyone should up their dosage of Vitamin D. People should be tested for both the active form (Calcitriol 1,25(OH)2 D) and the “prohormone” form (Calcidiol 25 (OH)D). I hardly ever see the Calcitriol form tested by physicians, but it should be tested and I will explain why in a followup post. There is likely a ‘sweet spot’ for each person, but for a chronic urticaria patient it seems 4000IU/day is a good starting point. However when taking Vitamin D I would make sure to take one with Vitamin K2 as Vitamin D supplementation can deplete Vitamin K (in addition there is evidence that it may deplete Vitamin A and Vitamin E as well).
Mediator Release Testing (MRT) and the LEAP elimination diet should absolutely be considered if taking Vitamin D in supplement form does not help ameliorate the symptoms. I would consider MRT/LEAP for anyone with other symptoms in addition to the urticaria (acute or chronic), such as digestive, nasal, joint pain, or emotional symptoms. In the case of chronic uritcaria, autoimmune diseases are often triggered by food antigens. The MRT food sensitivity test can accurately determine (with >90% specificity and sensitivity) which foods are triggering inflammatory responses. In addition I would consider embarking on a gluten free or at least a wheat free diet (but first ruling out Celiac disease) as there is a lot of evidence that gluten plays a significant role in many autoimmune conditions. So often taking away the offending foods can quickly eliminate symptoms such as hives.
As you can see there are many non pharmaceutical options available for urticaria sufferers. As with many chronic issues in today’s world both diet and nutritional status can play a role and the solutions can often be simple. There are other nutritional imbalances to look at with urticaria, such as magnesium deficiency or something known as methylation status. But the above is an excellent starting point.
Yours In Health,
George Mandler CNS CLT LDN LicAc
References
Grzanka A, Machura E, Mazur B, Misiolek M, Jochem J, Kasperski J, Kasperska-Zajac A1. Relationship between vitamin D status and the inflammatory state in patients with chronic spontaneous urticaria. J Inflamm (Lond). 2014 Feb 3;11(1):2. PMID: 24484740. [PubMed] [Read by QxMD]
Rorie A1, Goldner WS2, Lyden E3, Poole JA4. Beneficial role for supplemental vitamin D3 treatment in chronic urticaria: a randomized study. Ann Allergy Asthma Immunol. 2014 Feb 5. PMID: 24507460. [PubMed] [Read by QxMD]
Goetz DW. Idiopathic itch, rash, and urticaria/angioedema merit serum vitamin D evaluation: a descriptive case series. W V Med J. 2011 Jan-Feb;107(1):14-20. PMID: 21322467. [PubMed] [Read by QxMD]
Kasperska-Zajac A1, Brzoza Z, Rogala B. Sex hormones and urticaria. J Dermatol Sci. 2008 Nov;52(2):79-86. PMID: 18485675. [PubMed] [Read by QxMD]
Zuberbier T1, Chantraine-Hess S, Hartmann K, Czarnetzki BM. Pseudoallergen-free diet in the treatment of chronic urticaria. A prospective study. Acta Derm Venereol. 1995 Nov;75(6):484-7. PMID: 8651031. [PubMed] [Read by QxMD]
Maintz L1, Novak N. Histamine and histamine intolerance. Am J Clin Nutr. 2007 May;85(5):1185-96. PMID: 17490952. [PubMed] [Read by QxMD]